Minimizing transplantation risks
Erlangen Scientists decipher how dangerous inflammations develop after stem cell transplantation
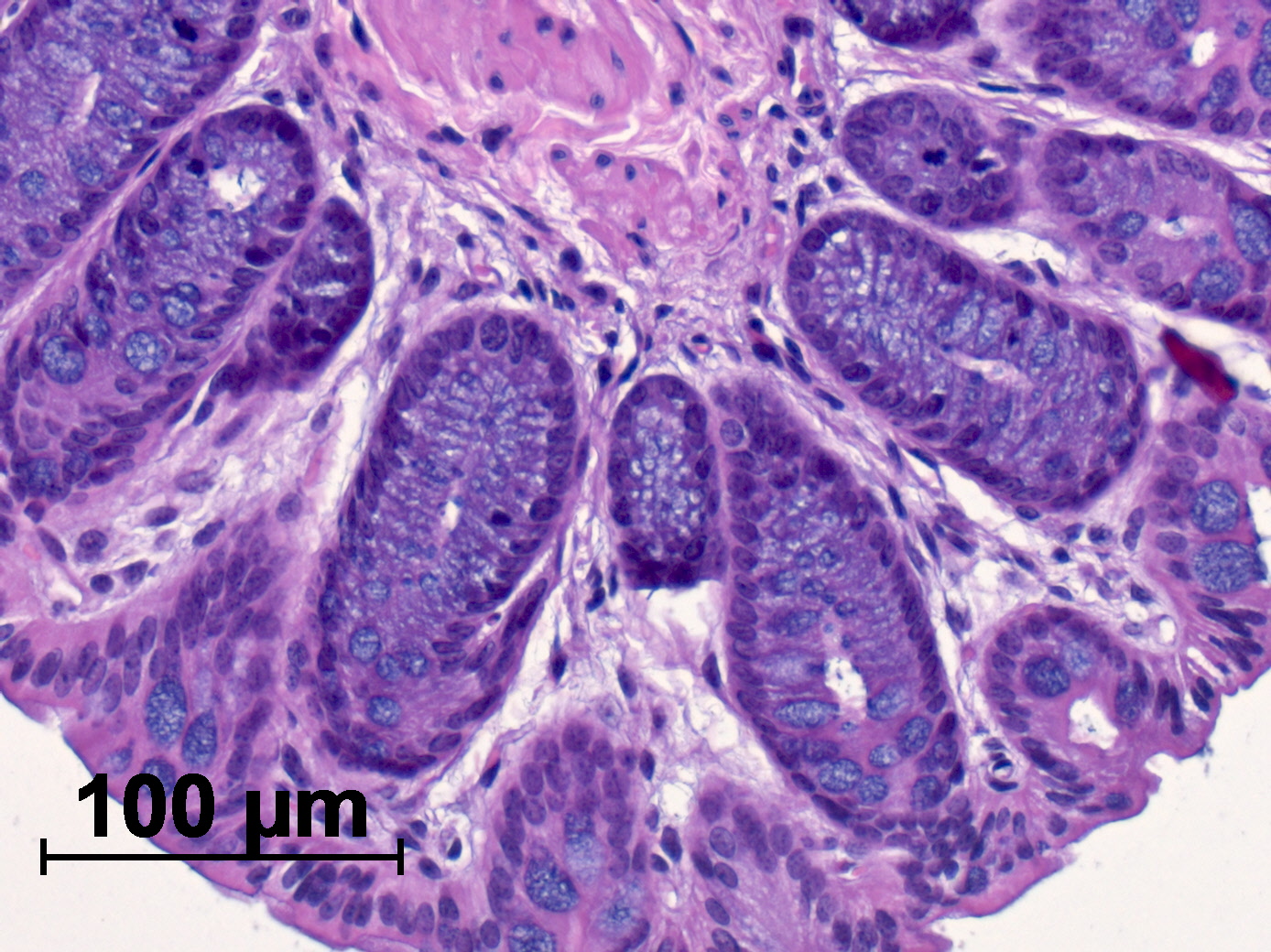
Often, bone marrow transplantation is the salvific therapy for patients with leukaemia, but the risk of complications is high. Despite the time-consuming and often lengthy search for a suitable donor, almost half of the patients suffer from an unwanted reaction of the immune system, which is often directed against the skin and liver and in up to 50 percent of cases against the intestines. Researchers from the University Hospital Erlangen and the Friedrich-Alexander-University of Erlangen-Nuremberg (FAU) have now been able to decipher how these inflammations of the intestines, which are sometimes life-threatening, occur and show a possible treatment approach. Their results have been published in the Journal of Clinical Investigation (DOI: 10.1172/JCI89242).
The violent immune reaction is triggered by a special form of the donor’s defence cells. These so-called T-lymphocytes recognise the recipient’s body cells as foreign and attack them. The researchers from Erlangen have now shown that this special form of T-lymphocytes is controlled by a protein called BATF (basic leucin zipper ATF-like transcription factor). “The BATF protein works like a central switch in the donor T-lymphocytes,” said Prof. Dr. Kai Hildner from the Department of Internal Medicine 1- Gastroenterology Pneumology, Endocrinology (Director: Prof. Dr. Markus F. Neurath). “If the protein is switched on, highly aggressive immune cells can develop, which massively intensify the inflammatory processes and then, in interaction with other immune cells, cause great damage to the intestine after stem cell transplantation.”
The group led by Professor Hildner in cooperation with the Department of Internal Medicine 5 (Director: Prof. Dr. Andreas Mackensen) of the University Hospital Erlangen and working groups in Frankfurt, Regensburg and Würzburg were able to prove another connection: The T-lymphocytes of the donor release a messenger substance (GM-CSF – granulocyte-macrophage-colony stimulating factor) and mediate the inflammatory reaction in the intestine. If the researchers blocked the development and function of these specialized T-lymphocytes with drugs, the inflammations in the intestine disintegrated.
The scientists hope that the discovery of this molecular mechanism will enable them to develop new therapies for influencing inflammation of the intestinal tract after transplantation in order to further increase the survival chances of patients after stem cell transplantation.
Manuscript:
https://www.jci.org/articles/view/89242
Further Information:
Prof. Dr. Kai Hildner
Phone09131 85-35908
E-Mail: kai.hildner uk-erlangen.de
uk-erlangen.de
Source: uni | mediendienst | forschung Nr. 4/2018 vom 7. Januar 2018